Hi! My name is Kyle Hornby and I'm a Family Dentist providing Root Canal Treatment in Kitchener and Waterloo. In today's blog post, I'd like to demystify root canal treatment while dispelling some of the myths and misconceptions out there.
Without delay, here are the 10 most frequently asked questions surrounding root canal treatment.
We encounter many patients who think that they lose some or all of their root during treatment. Importantly, the root(s) anchor your teeth in jawbone. This allows your teeth to have support when chewing food. So, you really need to keep your roots at all costs.
Luckily, root canal treatment cleans the soft tissue, nerve, or dental pulp from inside of your roots, while leaving the roots themselves intact. The point of doing this is to either get access for cleaning bacteria out, or to remove nerve tissue that has become unhealthy, inflamed and painful.
So, when you hear a friend or colleague telling others that their root canal treated tooth has no roots, you can gently correct them!
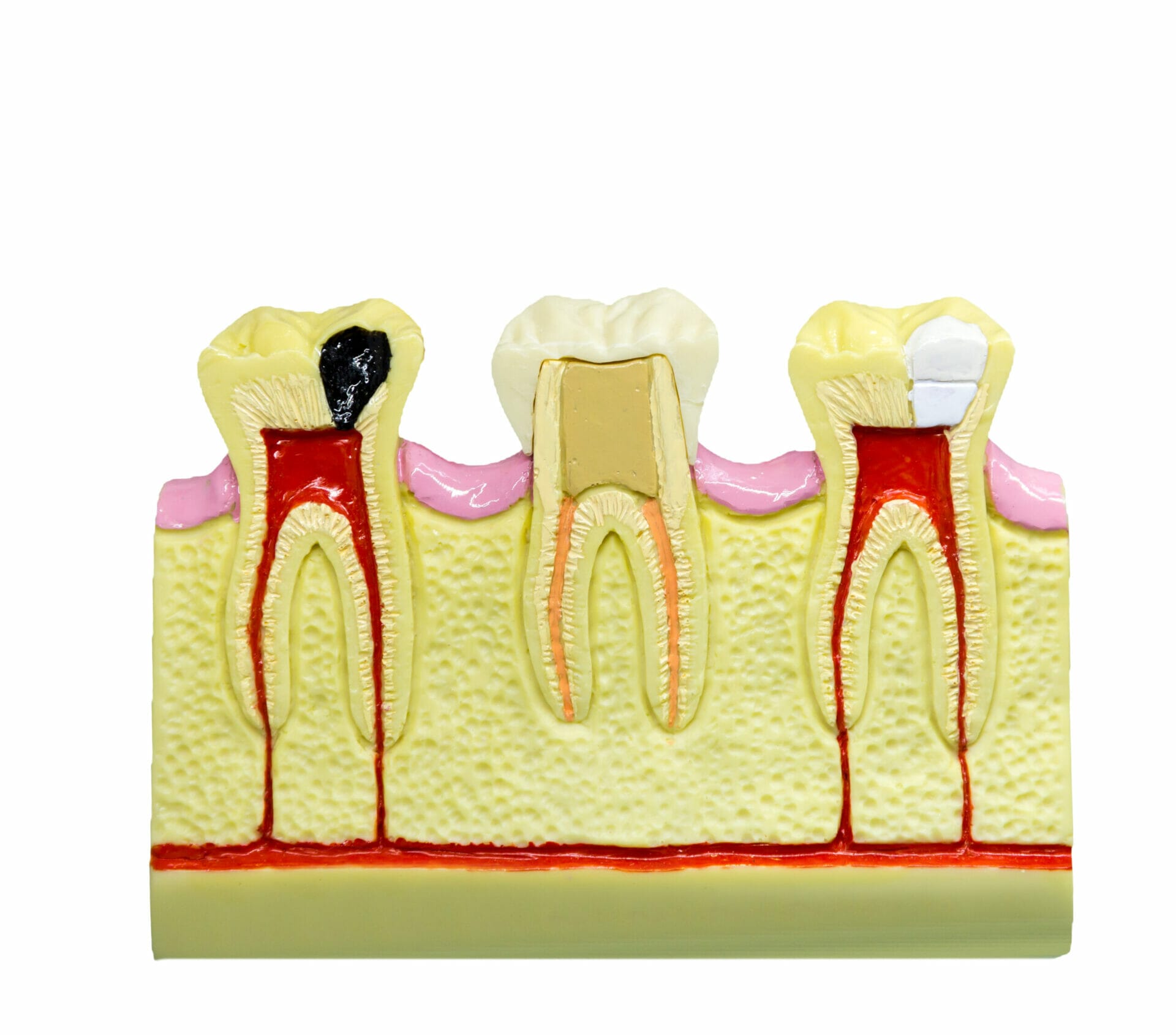
The most common reasons for root canal (Endodontic) treatment are infection of the inside of your tooth (the dental pulp) or unremitting pain due to an inflamed and hyper-responsive nerve (often called a "toothache").
Patients needing Endodontic treatment often present to us with pain on chewing, a deep cavity that has allowed bacteria into the nerve space or dental pulp, or a persistent toothache that won't settle down. (In some cases, a past dental filling placed close to your nerve can trigger root canal treatment much later on).
Sometimes a fractured tooth can only be rebuilt properly if anchored down inside the roots by a post. To achieve this, your Dentist will need to first complete root canal treatment to gain sterile access for post placement. This is a much rarer indication for root canal treatment.
Root canal treatment removes nerve tissue, and blood vessels and capillaries from your tooth. Sometimes this tissue is living but in many cases (such as an infected tooth or dental abscess) these tissues are dead or necrotic already.
While a root-canal-treated tooth is technically dead or non-vital, you can still perceive chewing pressure with your tooth. This is because there are millions of tiny nerve fibers in the Periodontal Ligament that wraps around the outside surface of your tooth roots.
Interestingly, the answer is no. In some cases, a painful or infected tooth requiring treatment my have a calcified pulp or nerve. This occurs when the soft tissue in the root canals becomes hardened over time. In these cases, it may not be possible to complete the necessary treatment and, instead, tooth extraction will be the only option.
Occasionally, your Dentist will refer you to a Endodontist for a 2nd opinion. This will enable them to give you information on the likelihood of successful endodontic treatment.
This is probably the biggest misconception surrounding root canal treatment. Endodontic therapy, in fact, relieves existing pain due to an inflamed or infected dental pulp (nerve). Local anesthetics can effectively numb your tooth so that you can have treatment completed comfortably.
With any treatment, communication is key! If you are experiencing sensitivity during root canal treatment, simply tell your Kitchener Dentist so that they can provide supplementary local anesthetic.
After treatment, you may experience tenderness in response to pressure or chewing. This is more likely if treatment was needed to resolve a painful dental abscess. If post-operative pain exists, it typically resolves within 2-3 days and can be minimized by anti-inflammatory medications.
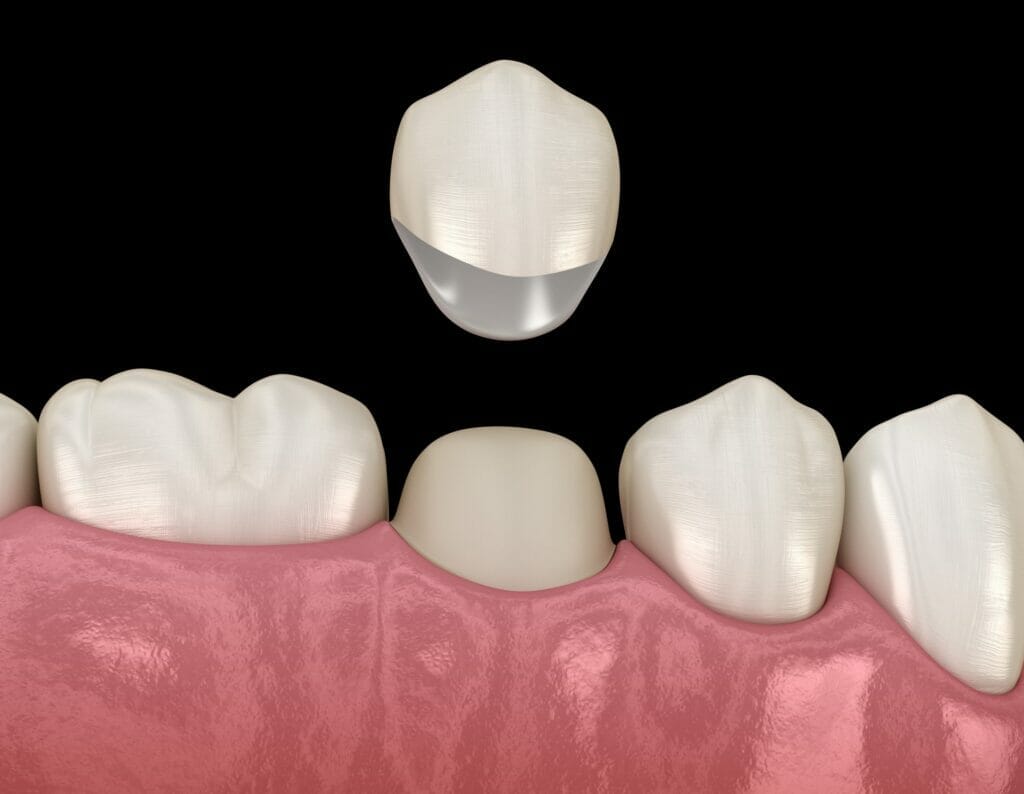
Your Kitchener Dentist will recommend a crown after completing Endodontic treatment. The treatment itself resolves inflammation or infection of the dental pulp. However, post-treatment, your tooth will be more brittle and susceptible to fracture.
How can you minimize this risk?
Placement of a dental crown will reinforce and protect your endodontically-treated tooth. Crowns are like helmets, and they can help your teeth to absorb the daily rigours of chewing food without any unwelcome outcomes.
Yes, root canal treatment can certainly fail. In fact, I see many patients each year who note that they themselves, a friend, or a family member had endodontic treatment that didn't hold up, long-term. There are a number of reasons for this.
Most commonly, a tooth will become re-infected after treatment. This may occur 8 months later or it may occur 15 years post-treatment. The most common cause of reinfection is an incomplete initial treatment.
Your Dentist must reach the end of your root canal or tip of the root(s) to achieve a fully cleaned space. Occasionally, we see patients whose root canal treatment failed and the cleaning and filling of the root is clearly "short". That is, the entire length of the root canal was not reached and cleaned.
Another reason for endodontic failure is cracking. Specifically, your tooth may be cracked prior to treatment allowing leakage of contaminants and bacteria into your jaws. This results in infection or abscess. If one or more cracks aren't detected, this can lead to trouble, symptoms of pain, and re-infection later on.
What can be done if treatment fails?
That's a great question.
In some cases, a re-treatment is possible to clean and re-sterilize the root canal system. Where this is not possible, tooth extraction is the only option for treating infection.
If your tooth is extracted, you can replace it with a dental implant, denture, or dental bridge.
Generally, thorough root canal treatment provides good longevity and allows you to keep your tooth. Unfortunately, there are some examples of incomplete treatment floating around out there. When those treatments fail, patients often assume that root canal treatments just don't work.
If I wasn't equipped with the dental knowledge that I have, I'd draw the same conclusion, too.

No. There is absolutely no sound evidence or peer-reviewed research showing that root canal treatments cause cancer. In fact, Endodontic treatment eliminates infection and a source of bacteria than can enter your systemic circulation contributing to an array of other health issues.
Root canal treated teeth can discolour and this often results from a pulpal hemorrhage that occurred during treatment. When your Dentist accesses a vital (live) dental pulp, it bleeds. If some blood is left behind following treatment, it can cause discolouration of your tooth over time.
Discolouration can also occur in a tooth that needed root canal treatment following an impact or trauma injury. These teeth discolour because of the impact (such as a fall or sports injury) sustained and not necessarily because of a completed root canal treatment.
Common colours include black, purple and grey. If this occurs, you can crown your tooth or undergo a simple process called internal bleaching or tooth whitening to eliminate the persistent staining.
Root canal re-treatment is an option where an initial root canal treatment has failed. Root canal re-treatment usually comes in 2 flavours: a simple re-do of the initial endodontic treatment or apicoectomy.
The straightforward re-do involves dissolving the Gutta Percha rubber filling material inside the root canals, followed by a repeat disinfection. Your Endodontist will then re-fill or re-seal the canals.
An apicoectomy is typically done if your Endodontist feels they cannot re-access the entire canal system. This makes a simple re-treatment impossible to complete. In an apicoectomy, the Endodontist will access the root tip through a small hole in the gums and then they will shave off the infected root tip. They then stitch the gums closed and any infection will heal allowing further use of your tooth.
You can learn more about root canal treatment by visiting the American Association of Endodontists website, here.
By Dr. Kyle Hornby, Kitchener Dentist
Our Dentist Office in Kitchener is conveniently located Downtown. We are a short drive away for families in Waterloo, Breslau & St. Jacobs. Our central location means we truly offer family dentistry near you!
This article is not intended to be a substitute for professional advice, diagnosis, or treatment. Accordingly, always seek the advice of your Dentist or other healthcare providers regarding a dental condition or treatment.
Services
Routine Dentistry & Tooth Repair
Oral Surgery & Tooth Removal
Prosthetic Dentistry & Tooth Replacement
Protective/Preventive Services
Teeth Whitening
Schedule an Appointment Now