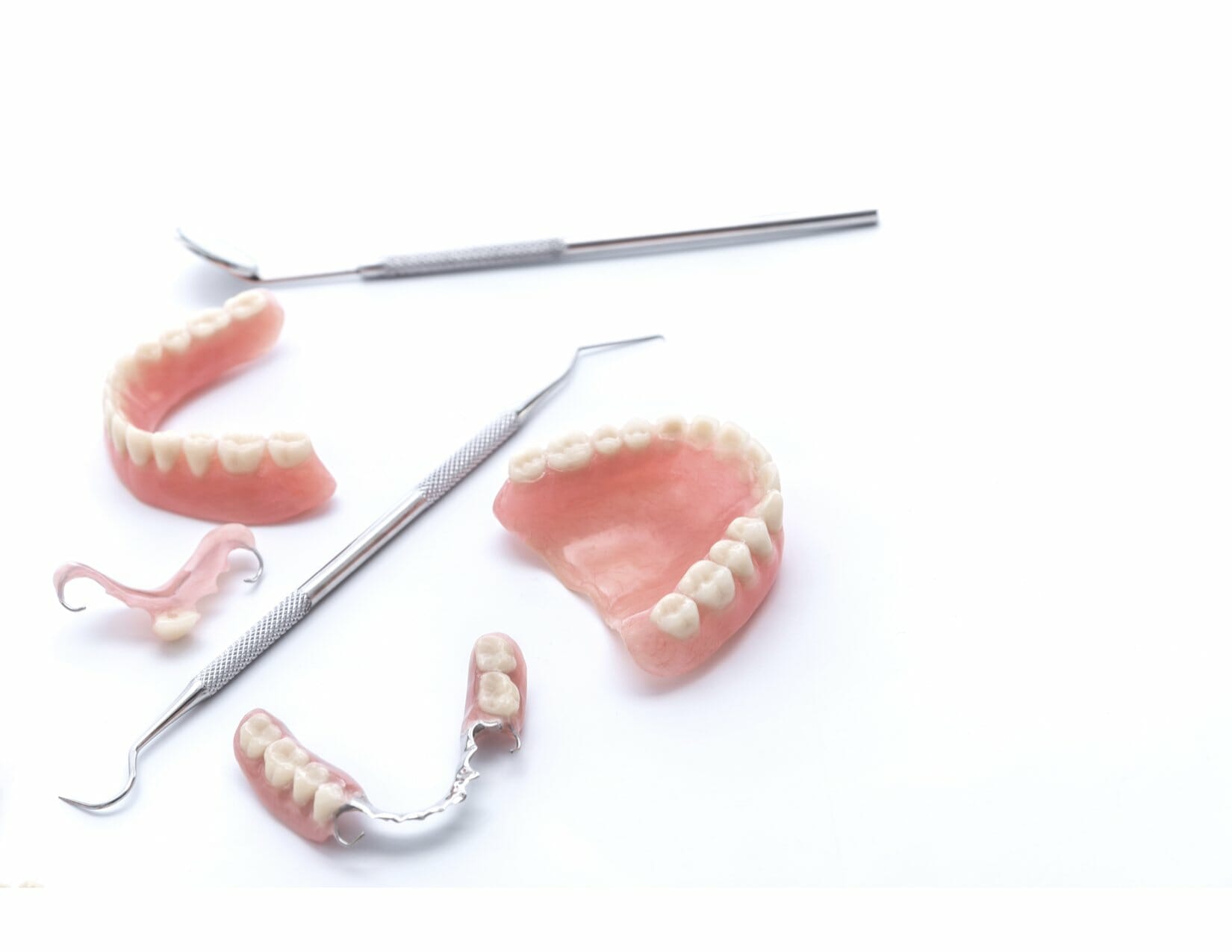
Are you considering or pursuing Dentures in Kitchener, ON? I have written this article to provide a comprehensive guide to complete and partial dentures. If you read this before discussing denture options with your Kitchener Dentist, it will help you to better understand dentures. I sincerely hope that you find the content useful!
Estimates suggest as much as 8% of our North American population wears complete dentures. Another 10-12% of people are wearing partial dentures. Many of these people visit their Dentist each year to address problems regarding denture-related soreness or poor fit. It is important that patients understand the strengths, weaknesses, and limitations associated with partial and complete dentures. This knowledge is not commonly available to them. Fortunately, having this knowledge will help them to better understand the underlying reason(s) for their problems. Moreover, a sound understanding of how dentures work and what conditions are required for their success will empower patients to better pursue adequate solutions in denture treatment.
I have organized all frequently asked questions into categories below. It may be useful to scroll the list first so each section heading can guide you to the right information. The sections I have used are based on different chronological points along the denture adventure:
1. initial phases that include gathering basic knowledge and thinking about making the transition to dentures; 2. secondary phases including actively pursuing treatment information and denture providers; 3. adaptation phase for early denture-wearers pursuing information on cleaning & maintenance of their appliance and; 4. the troubleshooting phase where patients may need information related to denture improvement/adjustment and repair.
Table of Contents

Complete dentures and partial dentures vary in composition. Even partial dentures on their own can very in composition. Below I outline materials used in the fabrication of each:
Complete Dentures. Complete dentures are made entirely of acrylic. Both pink gum segments and the denture teeth themselves are made of acrylic. Acrylic is a durable material that is lightweight. Because of this, it won’t interfere with suction-based retention like a heavier material might. Some implant-retained dentures are made of porcelain. This is a highly esthetic material but it is brittle (think chipping and fracturing) and much heavier compared to acrylic. Porcelain dentures are also significantly more costly compared to acrylic complete dentures.
Partial Dentures. Partial dentures also come in two main varieties: Cast Metal Base and Acrylic Base. Although acrylic-base partial dentures do contain a small amount of metal (for the retentive arms or clasp that clip onto natural teeth) cast-metal-base partial dentures contain much more metal. A cast metal denture has a base or framework made of metal alloy containing primarily cobalt and chromium. Occasionally, the alloy contains nickel but is becoming less common due to the prevalence of nickel-based allergies. Pink denture acrylic is set over the metal alloy (although some portions of polished metal may remain exposed). Teeth are made of acrylic or resin. Cast metal partial dentures are far more durable compared to acrylic-base partial dentures.
An acrylic-base denture is made primarily of acrylic with no metal framework or skeleton. It will, however, typically have metal arms or clasps that clip onto natural teeth for retention. The teeth are made of either acrylic or resin. Acrylic-base partial dentures are lighter in weight and less expensive compared to their cast metal variation. Acrylic dentures, however, are more prone to cracking and fracture.
Immediate Complete Dentures are a treatment option that enables patients undergoing full arch extraction (or removal of all remaining teeth) to have teeth right away. In some scenarios, patients wait 5-6 months for gum healing and stability before pursuing dentures. In contrast, immediate complete denture patients have a prosthesis in place minutes after dental extractions. So, what are pros and cons associated with each strategy?
Pros:
Cons:
Pros:
Cons:
Valplast dentures are made of a flexible resin base providing the ability to bend and deform your denture slightly. Valplast is typically only used for partial dentures because of limitations associated with forming and cooling this material. The major advantage of Valplast over acrylic is in its flexibility. Flexibility allows greater denture tightness. When acrylic is too tight, a denture can't full seat. Valplast, however, can deform slightly to slide over teeth and lock into place.
Complete dentures and partial dentures differ in terms of how they stay in place in your mouth. Partial Dentures have metal clasps or arms that clip around some of your remaining teeth to lock firmly in place. Complete dentures do not have this luxury. With no teeth remaining, the Complete Denture uses suction to stay in place. When you moisten the underside of your denture and seat it firmly against your gums, most air is pushed out. This creates a vacuum seal and “suction fit”.
Most patients can reliably generate suction with an upper complete denture. In comparison, it is very difficult to generate suction with a lower complete denture. This is because of the large void or cut-out prepared to accommodate space for your tongue. Often times, a patient will need to use a denture adhesive to better keep their lower denture in place. In cases of severe jawbone loss, the patient might need to have implants placed to retain their lower denture. So, dental implants provide yet another mechanism by which complete dentures stay in place. Though more commonly used to retain lower complete dentures, dental implants can also be used to retain or support upper complete dentures.
Dentures do not prevent bone loss. Natural teeth absorb forces from their top-third (the crowns on which we chew) down through their lower two-thirds (the roots). This regular force acts to stimulate the periodontal ligament and jawbone surrounding the roots. In doing so, it activates a mechanism which preserves and maintains jawbone over time. Without tooth roots and regular stimulation of the deep layers of the jawbone, loss of bone volume occurs. In fact, the compressive forces exerted by dentures during chewing may even act to accelerate bone loss over time. As bone is lost, overlying gums change shape and gaps develop between the oral tissues and the underside of your denture. This process may necessitate periodic relining your denture to re-establish proper fit and retention.
The short answer is, YES. This effect is much greater with an upper denture because it covers the palate, and the palate contains lots of machinery for smelling and tasting things. This machinery exists in a lower density in other parts of the mouth so, technically, anything that covers soft tissue in the mouth will diminish your ability to taste foods to some degree. Additionally, partial dentures can contain parts composed of metal alloys and these will have a faint taste to them that may influence how your food tastes.
This is a very common concern that we hear from our patients. Every denture, whether partial or complete, has an acrylic component that interacts with the gums. Because of this thin layer of acrylic, your tongue now has less space to move around and will contact gum tissues or the roof of the mouth sooner during speaking. This is most noticeable with an upper complete denture because it covers the roof of the mouth (this is where you place your tongue when making “s” sounds). As a result, patients often notice a lisp or having their “s” sounds come out more like soft “th” sounds. Luckily, most patients make the necessary adjustments and this lisp is gone within 1-2 weeks.
Dentures are a cost-effective way to replace many missing teeth. They can also provide a very aesthetic result to patients looking for a beautiful smile. There are a few keys to achieving a beautiful smile with dentures:
Complete dentures must cover a large surface area to generate suction and provide support for chewing. Unlike partial dentures, they typically extend far into the trough where the gums attach to the cheek. So, denture acrylic can be felt when you put light pressure on the skin all around the lips. Due to the thickness of the acrylic, most people will find a slight puffiness to their lips when dentures are in place. Unfortunately, there is no way to avoid the thickened or puffy appearance of the lips. This is because your dentures need to have a certain thickness of acrylic to be strong and fracture-resistant. If you are a partial denture wearer, the appliance is not likely to change your appearance in any way.
For the most part, yes, dentures can be comfortable. The key factors for producing a comfortable denture are:
1. The denture has been well made and has been adjusted where necessary. Where a denture has been made from poor or distorted impressions, the fit is likely to be imprecise, and the result will be an uncomfortable denture. If the denture border is overextended, it will exert excessive pressure on soft tissues causing tissue ulceration and pain. If heavy spots underneath the denture are not shaved down or “relieved”, he gums will become ulcerated resulting in pain.
2. The patient has enough jawbone to provide adequate support and allow for suction and retention. Most patients I see who have very little remaining jawbone find their denture moves when eating and so, sadly, they function in pain and discomfort. In contrast, patients who have plenty of residual jawbone can function with their denture adequately and in relative comfort.
3. The patient has firm and immobile gum tissue. As I have mentioned in other sections, excess or “redundant” gums can be very mobile and so anything that rests on top of them (i.e. a complete denture) will move and shift as well. The movement, again, causes friction and irritates the gums causing pain and discomfort.
4. Additional forms of retention.
A patient whose denture is retained by dental implants or who has a partial denture that locks into place around natural teeth will enjoy a much more comfortable denture-wearing experience compared to patients wearing a basic complete denture.
When exploring Dentures in Kitchener, ask your Dentist if the anatomy in your mouth will support a great treatment outcome!
Complete dentures and partial dentures can be made by a Denturist or they can be made by your Family Dentist. Both practitioners can provide you with well-made, affordable dentures. It is important to note that all Denturists make dentures while only some Family Dentists provide this service. A limited number of Dentists will provide both surgical services (tooth extraction and bone grafting) as well as denture fabrication. This is very convenient for patients as they can have all treatment completed comfortably in one place. There may be cost differences between services provided by a Dentist and Denturist. It is important for you to ask your Family Dentist if they can make dentures for you and to discuss costs in advance of treatment. In some cases, a Dentist and Denturist will work together on more complex cases to provide an expert result.
Some dental plans cover procedures deemed to be “major” or “non-routine” dental care. Like dental crowns, dental bridges and dental implants, dentures fall under this category. You can find out about your insurance coverage for dentures by contacting your insurance company, reading through your dental insurance booklet or manual or by having your Kitchener Family Dentist send a pre-determination or cost estimate to your provider. If your dental insurance provider does not cover dentures, then plan on an out-of-pocket expense of roughly $1500 (not including costs of related extractions or relines).
This is a really interesting question, so much so in fact, that Dentists will likely differ on their answer to this question.
Generally speaking, you can generate good suction and retention (or resistance to movement or loosening) with an upper complete denture. Accordingly, if you are hanging on to 3-4 remaining teeth that likely won’t last, it is probably better to extract those teeth and have a complete denture made. This course of action would likely give you a better functional result than keep 3-4 teeth to anchor a partial denture. Additionally, this strategy would prevent you incurring future financial costs associated with restoring and treating teeth with a poor prognosis.
If you are pursuing Dentures in Kitchener, ask your Kitchener Dentist whether a complete or partial denture would be a better fit for you.
While many people might think that Dental Implants are easily superior to Dentures, it is not necessarily the case. I think this question is very useful because providing an answer requires that I dive into lots of useful facts about both options. In doing so, I hope to provide you with a greater understanding of your treatment options.
Dentures, whether complete or partial, provide a cost-effective solution for producing multiple missing teeth. There is an appeal to knowing that you can replace lots of missing teeth for roughly $1500. Additionally, denture costs do not increase as a function of the number of teeth they replace. More simply, an 8-tooth denture does not cost twice as much as a 4-tooth denture – as you replace more missing teeth with a denture the additional cost for each added tooth is very small.
As a guideline, I would say that an 8-tooth denture might cost $60 – $75 more than a 4-tooth denture. This is because the patient is only charged for the cost of additional teeth and any extra material used to build a larger framework or base. Dentures can also be modified over time in a very cost effective way. As gums change shape, retention may deteriorate, but, luckily, a $300 – $400 reline can fix the problem. As conditions in the mouth change, dentures can be modified or adapted easily to these changes.
When considering a complete lower denture, it is important to think about its shape and coverage. A lower complete denture is shaped to give space for the tongue (whereas an upper complete denture can cover the entire palate) and so you have a shape and design that cannot generate suction with the soft tissues and gums. Because of this, it is often a better strategy to keep 3-4 remaining lower teeth (or hopefully more than that) to anchor a partial denture. Even if doing so gives you only 5-10 years of function before remaining lower teeth are lost to dental decay, fracture or gum disease, the strategy enables you to prolong need for a lower denture. This is important because, again, you cannot generate suction and/or good retention with a lower complete denture typically.
So, upper complete dentures typically provide reliable retention and function while lower complete dentures do not. Accordingly, a lower partial denture scenario (where possible) is likely to be superior to having a lower complete denture. Conversely, in scenarios where few teeth remain, dental extraction followed by placement of a complete upper denture is likely to provide a sound and functional result. These are not steadfast rules, however, and it is important to discuss all available options with your dental professional.
Partial denture prices can vary based on composition. Removable partial dentures come in two different types: Cast Metal & Acrylic-Only. Accordingly, there are 2 price ranges for partial dentures that correspond with the materials used to make them. A partial denture with a cast metal base typically costs $1,300 – $1,500. A partial denture with and acrylic-only base is less durable in comparison but costs approximately $600-$900. Fees are typically dictated by the Ontario Dental Association Fee Guide however, a portion of the cost is for dental lab work and materials and this amount can vary depending on material used, size of denture, number of teeth replaced, etc., If you are pursuing Dentures in Kitchener, you should discuss fees with your Kitchener Dentist prior to embarking on treatment.
Complete dentures are made entirely out of acrylic. In Kitchener, Complete Dentures typically cost $1,400 – $1,500. Price can vary slightly depending on whether the denture is placed immediately following dental extractions or if it is fabricated for a healed and stable arch. This is because and immediate denture will be supported by gums that continue to heal from extractions for 4-6 months. Thus, a reline or reshaping of the denture surface is required for proper adaptation to the fully healed, stable gum tissue. A denture reline costs approximately $500.
Toothpastes contain small abrasive particles for disrupting and removing biofilm, plaque and tartar. These abrasives are generally not destructive against tooth enamel to any significant degree. Denture acrylic, however, is much softer than enamel and so brushing your denture with toothpaste is likely to cause wear lines on, and roughening of, your denture.
Dentures can be soaked overnight in cleaning solutions designed to minimize stain, tartar/plaque buildup, and bacterial deposits. These solutions can be purchased at most pharmacies and drug stores and are offered by manufacturers such as Poligrip and Polident.
You should adopt a habit of cleaning your dentures at least once a day. The most convenient time for this is at night when you should remove your dentures to allow for “rebound” or relief of your gums. You can place your dentures in a tablet-based cleaning solution such as those offered by Poligrip or Polident. This will dissolve plaque, hard tartar, stains and remove bacteria so that your denture does not become contaminated and unsightly over time.
So, here’s the thing: there are expensive solutions and there are inexpensive solutions and, to some degree, you get what you pay for. If you find that your denture is short on suction and won’t stay in place, a denture adhesive might increase retention. Many adhesive products are paste-based (like Fixodent denture adhesive or Poligrip denture adhesive) but some, like Sea-Bond, are mesh-based and are much tidier. I find my patients are happy using Sea-Bond to ramp up denture retention.
Another option is to have your Family Dentist, or Denturist, evaluate the fit of your denture. If your denture is 5 years old or more, you may have developed gaps between the denture and your gums (which do change shape slowly as you lose bone over time). A reline can fill these gaps with a soft impression material and a dental lab can turn the soft stuff into hard acrylic within a day. Denture relines often improve the suction that you can generate between acrylic and gums. When suction increases, retention increases (and looseness decreases). A typical denture reline costs between $400 – $500.
If cost is not an issue for you, ask your Family Dentist about implant-retained dentures. Often times, 2-3 implants can be placed in the upper or lower jaw to enable “clipping-in” of your denture. While placing these implants and modifying your existing denture can cost $6,000 – $10,000, you are likely to find that your dentures no longer move or loosen during eating and the variety of foods that you can enjoy will increase significantly.
As a general rule, you should remove your partial or complete dentures before going to sleep. This allows your jawbone and gums to have some recovery time. Additionally, it allows for you to clean plaque and food debris from under and around your denture. Where complete dentures are left in the mouth indefinitely, fungal infections of the gums (such as candidiasis or “thrush”) are likely to occur.
One exception to the rule: where an immediate complete denture has been inserted on the same day as teeth are extracted, the denture should ideally be worn for 48-72 consecutive hours to protect healing gums and to enable the underside of the denture to “shape” the gums and jawbone.
In the majority of cases…YES! Most components of your denture can be modified, fixed, or replaced. If a tooth breaks off of your denture it can be replaced. If your denture acrylic cracks or separates, that can be repaired as well. Conveniently, if you have a partial denture and require extraction of one or more teeth, the lost teeth can be added to your denture. Lastly, if you break a metal arm or clasp, a dental lab can repair it. Most denture repairs can be completed same-day, so long as the patient is seen in the morning to enable 6-7 hours for work to be completed. At our office, we can typically return a repaired denture in the early to late-afternoon after seeing our patient before 10 a.m.
Yes and No. Denture teeth can be replaced to give a different appearance or alignment. And a complete or partial denture can be relined to change the shape of its underside. The reline is done to better adapt the denture to gums that have changed shape over time. Theoretically, this should improve suction and therefore retention (less movement and falling out) of your denture. Larger scale changes in shape will usually require fabrication of a new complete denture or partial denture. For instance, you cannot take a denture made for 1 person’s mouth and re-shape it to fit another person.
This is a common question patients ask – people are always looking for ways to improve the brightness of their teeth and the quality of their smile. Traditional whitening agents (most are peroxide-based) do not work on acrylic or resin denture teeth. The only way that you can have whiter teeth in your denture is to have the existing denture teeth replaced. This is a denture modification that can be done same-day in most cases. I have completed these modifications in the past for patients and often times we choose to upgrade to a higher quality aesthetic denture tooth with our modification. Patients are typically delighted with the outcome and find the modification to be worth the cost.
In most cases, the answer is yes. This is where it helps to have a partial denture with a cast metal base. Metal can be soldered to the exiting base or frame to enable addition of denture teeth as natural teeth fail and require extraction. It is more difficult to have teeth added to a partial denture with an acrylic-only base. Typically, repairs can be made to add teeth within the same day. Where tooth extraction is required, your family dentist can remove a broken or fractured tooth early in the day, take an impression and have your repaired denture returned later that afternoon. The typical cost for a repair involving the addition of teeth varies, but should range between $300 – $500.
There are a few reasons why this might occur:
Deterioration of fit over time.
Without natural teeth, you will lose jawbone slowly over time. As you lose more jawbone, gaps develop between your gums and the underside of your denture. Think about a suction cup that attaches a thermometer to your window. When the suction cup is barely in contact with your window, a large gap between the two surfaces exists. It is not until you push the suction cup against the window that you develop retention or suction. This is because the pressure you apply is improving the adaptation of the suction cup surface to the window, minimizing the gap in between, while forcing air out to create a vacuum seal.
When you moisten a denture and put pressure to seat it on your gums, you achieve suction and retention in the same way. So, when gaps are larger (i.e. an ill-fitting denture due to jawbone loss over a number of years), you lose suction and retention. A denture reline or re-surfacing of your denture can be used “update” the fit of your denture. This will improve its adaptation to your gums, minimize gaps and air pockets, and really ramp up the suction and retention you are experiencing. In rare cases, however, there is very little remaining jawbone and a reline might not help much if at all.
Soft tissue impediments.
Your denture should extend over enough gum tissue to distribute chewing forces and provide support. However, there should be buffer room or space from soft tissue structures like the lingual and labial frena. These are the very connective tissue strands that connect the gums to the cheek and lip and to the tongue as well.
If you push your tongue over the biting edges of your front teeth and down into the soft tissue trough or vestibule below the gums, you will feel the labial frenum at your midline. These frena are very dense and deformable, like elastic bands. When you make certain sounds during speaking or when they become activated during different facial expressions, the frena can become tense and unseat or “pop out” your denture.
Sometimes a minor denture adjustment can be carried out to accommodate these changes in tension and shape that occur with frena in different situations. That is, acrylic can be removed from the edge of your denture to create a larger “buffer zone” for the frena. This way, it can no longer cause an unseating action by exerting force on the edge of your denture. A very prominent frenum can be surgically adjusted in cases where drastic adjustments would compromise the strength and durability of your denture.
Excess or “redundant” gum tissues.
Following dental extraction (or tooth extraction), a patient’s gums can heal in different forms. In many cases, the gums heal to an ideal thickness and are firmly attached to underlying jawbone. Occasionally, gums will “over-heal” leaving excess gum tissue that is mobile because it is not firmly attached to underlying bone. This second type of gum tissue is not ideal for the denture wearer. “Redundant” gum tissues allow the denture more freedom to move. When dentures move around too much, suction is lost and the denture can become loose or fall out. Ideal gum tissues can be ensured by proper pre-prosthetic contouring at the time of dental extraction(s). After the fact, gum tissues can be improved by gum surgery or “gingivectomy”. In this procedure, excess gum tissues are trimmed away using a scalpel or by a laser gum surgery approach.
Insufficient supporting jaw bone.
This commonly occurs in patients who have lost many teeth at an early age and now wear a complete denture. Many of these patients will battle with loose upper and lower dentures for most of their life. When there is not enough jawbone to “hold” and support the dentures, something has to be done to increase retention.
There are two solutions to this problem: a) use of dental implants to retain the dentures and b) use of a block bone graft to re-build jawbone. Sometimes both solutions are required together when there is not enough existing bone to allow for placement of dental implants. Dental implants can be surgically installed, and a new or existing denture can be clipped to the implants through adapters. The implant-retention prevent unseating and loosening of your complete denture. Implant-retained dentures have become very popular in the last 10 years. Where only a block bone graft is performed (this is very rare), the increased post-healing bone volume once again allows for proper denture support and retention to be established.
There are a number of reasons why dentures can hurt:
1. Recent extraction of teeth.
If your Kitchener Dentist has recently extracted teeth, having an immediate denture in contact with healing sites can be painful. While it is critical to wear your denture(s) during healing, remove your denture(s) occasionally to give yourself a break. Also, your Dentist or Kitchener Denturist can gradually adjust areas of the denture that increase gum irritation. Your Family Dentist might even be able to add a soft liner to the underside of your denture for relief.
2. Poor denture fit.
If your dentures are not properly adapted to fit your gums they will move when you eat. This movement causes friction which can irritate your gums and cause pain. They movement may occur because of gaps between your denture and supporting gums. In many cases, a denture reline or re-surfacing will fix this.
Your dentures may also move too much when eating because of excess or “redundant” gum tissue. If there is too much loose gum tissue in the mouth, it can't hold your denture firmly in place. Typically, a surgical adjustment of the gums (called a "gingivectomy") can fix this.
3. Denture Over-extension.
When teeth come out, there is an inevitable loss of jawbone over time. As you lose bone, your denture seats down further. Eventually, its edges can dig into the soft tissue trough where your gums attach to your cheek. This is a very common area where ulcers develop due to friction and irritation from their denture. Luckily, your Kitchener Dentist can simply reduce the extension of the denture to provide relief, and the ulceration will heal.
4. Your denture is pushing on abnormal structures. Okay, so I don’t mean to call anybody “abnormal”. What I’m referring to are uncommonly occurring soft and hard tissue anomalies of the mouth. These anomalies can make achieving a comfortable denture fit tricky at times. Some individuals have bony lobes or deposits called “mandibular tori” (pronounced “Tor-eye”) on either side of there tongue. These are basically overgrowths of bone originating from the side or lateral inner wall of the lower jaw. When a denture seats and makes contact with these thinly covered bony protrusions, it can cause pain. These tori exist in about 5-10% of patients.
Other patients have a bony lobe on the roof of their mouth called a torus. An upper complete denture will rub against this deposit during chewing, causing severe ulceration and pain.
Some people may have enlarged frena or connective tissue bands that connect their gums to the cheek and lips. Everybody has frena, but in a small percentage of patients they are very prominent. These soft tissue features can act like a rubber band. When a denture-wearer bites down, denture edges push down on frena causing stretching. When they release that pressure, the frena regains its original tension causing pressure on, and sometimes loosening of, the denture. Additionally, when a denture-wearer smiles, laughs, or pronounces certain words these frena can tighten. This tightening can also cause loosening or even ejection of their denture.
Your Kitchener-Waterloo Dentist will be able to detect these structures and make necessary adjustments to enable a comfortable result.
This is probably the most important question to understand as a patient who is looking into a transition to dentures. Dentures are a cost-effective means for replacing multiple teeth. Whether you need to replace 7 teeth with a partial denture or an arch of teeth with a complete denture, you can do so for under $2,000. Contrast that with dental implants which cost $4,000 – $5,000 to replace a single tooth! This is the biggest positive or “plus” with denture solutions: they are more cost-effective than other available solutions.
Now, in terms of comfort, dentures cannot compare to other, non-removable solutions. That is, Dental Bridges and Dental Implants feel just like natural teeth. They don’t have acrylic, plastic or metal components that extend onto your gums and onto the roof of your mouth. They don’t affect your speech and diminish your ability to taste the foods you love. So, to say the least, it takes every patient time to adjust to their new partial or complete dentures. However, this is not the same as “feeling normal”.
Denture patients should be made aware that their denture(s) will not feel or function like natural teeth. Dentists are responsible for setting expectations for different treatments. Its' not fair to assume somebody will know about a big change that comes with a treatment option.
Fortunately, over time, denture-wearers forget how life was with natural teeth. So, the combination of them adapting to their new prosthesis and forgetting about “old times” with natural teeth results in most denture-wearers learning to function satisfactorily with their dentures.
Gums and jawbone continuously remodel over time. After healing from dental extraction, this remodeling continues at a very slow rate. But, all the small changes add up. This means that occasionally your will need to reline your denture to re-adapt them to fit your gums properly.
To complete a reline, your Kitchener Dentist adapts a soft putty or gel to the underside of your Denture. They then seat the denture in the mouth and use tension from the lip and cheeks to round off edges of the putty.
The reline material fills any gaps between the denture and your gums. Your Dentist then sends the denture and putty to a dental lab where they convert the soft putty to a durable acrylic.
So, how often should this be carried out? Well, we have patients who have well-fitting, retentive dentures at 15-plus years strong without a reline. Other patients require a denture reline every 5-6 years. The need for a reline is related to the volume of jawbone available for “holding” or retaining the denture (that is, patients with a large volume of remaining jawbone tend to need relines very infrequently). It is also related to the rate of bone loss over time and that differs between individuals.
The best answer is to let the performance of your denture be your guide. Relines are generally necessary only when fit and retention have deteriorated. If your denture has good suction-based retention and stays in place when you eat, you probably don’t need to think about a denture reline.
Your Kitchener Dentist can repair or adjust most existing dentures to improve fit and resolve discomfort. When denture acrylic cracks, your Dentist can repair it. If a denture tooth breaks or separates from your denture, you can add a new one. If the metal arms or “clasps” on your partial denture, that is repairable too. Legitimate reasons for remaking a denture are few.
In addition, most dentures undergo gradual fine-tuning adjustments over time. This includes trimming and polishing borders and fine-tuning the patient's bite. In many cases, your Family Dentist can make small modifications to improve fit or repair defects while preserving what has become a familiar appliance.
Patients often have to endure a period of adaptation to a brand new denture. This is the case even if they have worn a different denture previously. In my practice, we would only remake a denture if I could not improve fit issues with a simple reline. I might also remake a denture if a patient had issues with poor fit and they were thinking about changing to new denture teeth, too. In these rare cases, the modifications may cost almost as much as a new prosthesis. And, there is always value to having a “backup” denture. The only other conceivable reason for making a new denture would be damage rendering the denture un-repairable. I have yet to see damage to this extent in clinical practice.
Looking for a new family dentist or a second opinion regarding your existing denture?
Give us a call at Enamel Republic today or request an appointment here!
I am always happy to discuss treatment options and to share with patients services that we provide for surgical extraction, full-arch extraction, grafting and immediate dentures. It’s one of many specialist services we provide to our patients! We look forward to hearing from you.
This article is intended to promote understanding of and knowledge about general oral health topics. It is not intended to be a substitute for professional advice, diagnosis or treatment. Always seek the advice of your Kitchener Dentist or other qualified healthcare provider with any questions you may have regarding a dental condition or treatment.